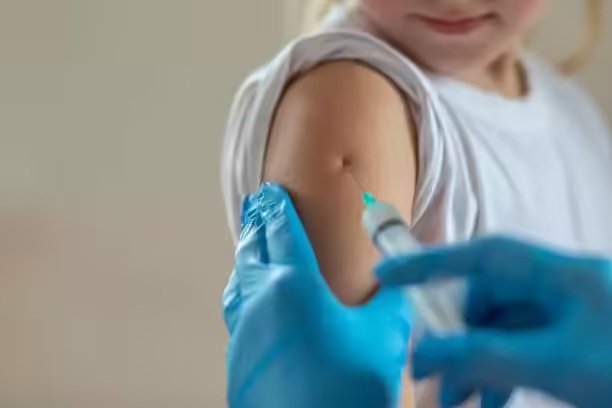
Breakthrough in Understanding Childhood Immunity to Strep A Could Accelerate Vaccine Development
A team of scientists has uncovered how young children naturally build immunity against Group A Streptococcus (Strep A), a bacterial infection responsible for up to half a million deaths worldwide each year. The finding could significantly speed up the creation of a life-saving vaccine. Strep A is a common bacterium that can cause mild illnesses like sore throat and skin infections, but in severe cases, it can trigger life-threatening diseases. While deaths from Strep A are rare in wealthier nations, outbreaks can be devastating. In late 2022, a surge in cases across the UK and Europe claimed hundreds of lives, including those of many children. The burden is far greater in low- and middle-income countries, where thousands die annually from the infection. Researchers from the University of Sheffield, working with the Medical Research Council (MRC) Unit The Gambia at the London School of Hygiene and Tropical Medicine, tracked how Gambian children acquire natural immunity. Published in Nature Medicine, the study identified specific antibodies linked to protection from Strep A, marking a crucial step toward vaccine design. The team observed that babies are born with some immunity passed down from their mothers, but this protection fades quickly. Young children, however, develop robust antibody responses to different components of the bacteria after repeated exposure. This discovery pinpoints a key window for immune development, which could guide more effective vaccination strategies. Lead researcher Dr. Alex Keeley said this is the first time scientists have seen in humans how antibodies generated through vaccination might prevent Strep A infections. Gambian scientist Fatouamta Camara described the infection’s “devastating burden” on communities and expressed hope that a vaccine could break the cycle of illness and socio-economic hardship. The research was a collaboration between Sheffield’s Florey Institute of Infection and the GSK Vaccine Institute for Global Health. Professor Thushan de Silva, who co-directed the study, emphasised the importance of cross-institutional efforts in delivering impactful global health research. Source: PTI